This is the third of a series of articles exploring the challenges and impact of overcrowding in various departments at Southlake Regional Health Centre in Newmarket, one of Ontario's most overloaded hospitals.
At Southlake Regional Health Centre's postpartum unit, new mothers can recover in a private family suite equipped with its own bathroom, a television, wifi, a fridge and microwave, and a pullout cot. The room is large enough to accommodate a support person and additional children comfortably.
Unfortunately, the suite isn't covered by OHIP.
Neither is a private or even semi-private room. What is covered is a room shared with two other new mothers.
Technically a unit for postpartum doesn't even exist — it was taken over two years ago by the medical program, said Sheena Shannon, manager of the maternal child and postpartum program at the Newmarket hospital.
Most neighbouring hospitals have renovated birthing units but Southlake's maternal child program hasn't seen much in the way of renovation in almost 20 years.
Even if it had been upgraded, there just isn't enough physical room to accommodate the steady increase in patients the hospital has seen in the past 30 years.
In York Region's newest hospital and in many others, private family suites are standard for postpartum patients, whereas at Southlake a postpartum private room can be hard to come by even if a patient is willing to pay for it.
"Depending how busy we are, (patients) might want a private room and we just don't have that capacity," said Stephanie Simson, manager of pediatrics and the neonatal intensive care unit (NICU).
What's left is a three-bed standard room with curtain dividers.
"If you have three mummies and three daddies and three cribs and all the equipment people bring in like car seats, it's really quite congested. I'd say it's probably dangerous because people can fall over things. We have to be very careful and strategic in where we put things. It's a challenge," said Shannon.
There are only eight beds for postpartum patients and the overflow are sent to the pediatric unit. If a private room isn't available, those patients also get moved to pediatrics.
With 2,600 deliveries a year, "it can be quite tight," said Shannon.
"It's like a chess game. Who needs what coverage and where can we go and then we're moving people around all the time, which just uses up resources and time. In an ideal world, everyone would have a private room for themselves," she said.
A new mother with six-day-old twins started out in a birthing room and ended up in a semi-private room in pediatrics. Because she had twins, she didn't have to share the room and joked that she had found a loophole to securing a private room.
The babies' father, a relative and two bulky bassinets were in the room with the new mother. Even without a second patient, the room was already full.
Had there been a second patient with baby, the curtain dividing the two beds would be pulled closed — leaving one unlucky mother without sunlight.
"I couldn't imagine having to share. And just having the natural light here, otherwise we'd be enclosed. And their schedule would be different from my schedule for feedings," she said.
Before ending up in the semi-private room, the new parents used private insurance to secure a birthing suite. "And thank God we did," she said.
Paying the additional cost doesn't ensure a patient will get the suite because the rooms are available on a first-come first-deliver basis. "It was a race for who would deliver first," she said. Because she was having a C-section, she got the suite despite the fact that another woman arrived before her.
"It made a difference, the room makes a huge difference, you just have the space and quiet and everything else —to have to share that, it would've been so hard."
Because the postpartum unit is now home to adult medicine — often they're elderly patients waiting for long-term care — the nearby NICU is locked at all times due to past instances of patients wandering in.
"It can be unpleasant, there's people yelling and screaming sometimes it doesn't smell very nice either," said Shannon.
"It's not very pleasant for moms to come down here," she added.
"We're constantly looking at spaces and see how we can be more efficient to deliver the same care in the structure we have," said Simson. "We just don't have enough space for our patients."
At Southlake, the NICU is open concept. There are privacy screens but at new hospitals the NICU is made up of individual pods, something Dr. Madeline Drake, a neonatal doctor in the NICU and pediatrics unit, said is ideal.
The pods create a quieter environment for the babies and a private space for families to bond with the babies, which makes a big difference, Drake said.
The NICU can accommodate 12 babies but there have been as many as 17. A room filled with 12 babies plus 24 parents, staff and machinery is very "congested and loud," Shannon said, and it's a challenge to create a space where babies are as unstimulated as possible.
There are normally four nurses per shift each caring for three babies. More than 12 babies requires an additional two nurses per shift, which, Shannon said, is hard to sustain for a long period of time because part-time staff end up working full time hours and full-time staff work overtime, which can lead to burnout.
"The nurses are amazing. They step up, they come in, they stay late, they help, they're amazing" Drake said.
Peds, NICU, birthing or postpartum is the type of department that you either love or hate, Shannon said.
"And if you love it you'll be there for your whole career. You just know, it's just there in your heart. That's your purpose in life — to make sure these families have everything they need. So it's just what you do, it's part of you."
While the hospital has not been able to expand physically to meet the demands of the community, it is expanding in other ways.
Four years ago, the NICU became a level 2C, which means the unit can care for younger and sicker babies and provide an increased level of care. This way, said Drake, babies don't have to be transported to another hospital and they can stay closer to their moms and dads.
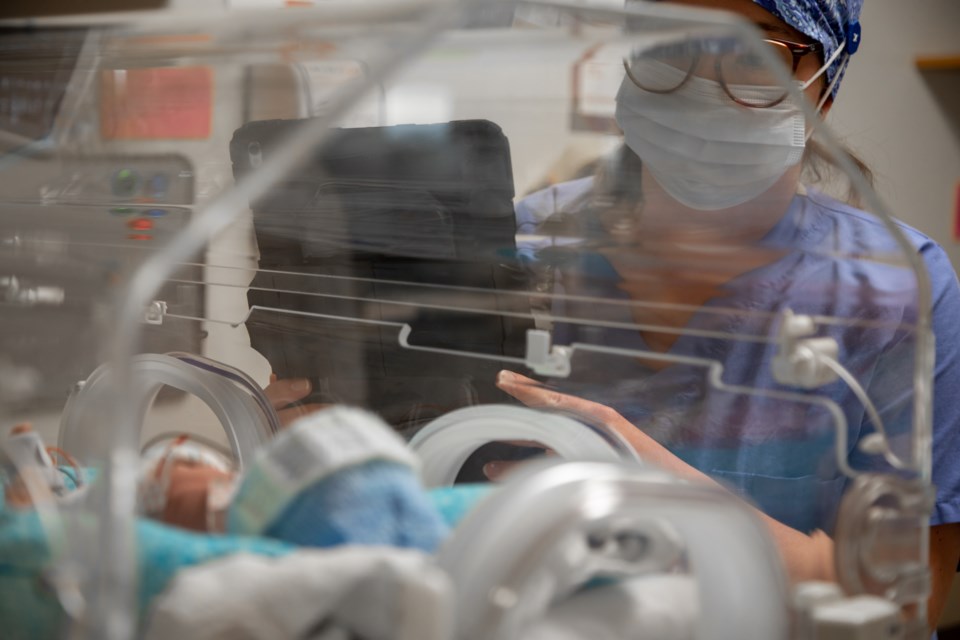
At the start of the pandemic, Southlake became the first hospital in Canada to implement AngelEye in the NICU. The program allows parents to receive real-time virtual updates on their baby's progress via photographs, texts and videos when they aren't able to be there in person.
In the fall, Southlake will join SickKids’ complex care program by becoming a satellite clinic. Nurse practitioners from SickKids will work with Southlake physicians to provide complex care to patients and eliminate the need to travel outside of their community for clinic visits.
"We're really expanding with the new clinics, lots of new pediatricians, we've expanded our program, the complex care clinics so we have all this potential it's just finding the space," said Drake.